


Sore throats are common, especially during flu season, and are often caused by minor infections or allergies. However, when throat pain occurs on only one side, it may signal a more specific underlying cause rather than a routine illness. Because the tonsils, lymph nodes, and surrounding tissues are usually affected equally, one-sided throat pain helps narrow the possibilities and can sometimes point to conditions that require prompt attention.
This guide covers the most common causes of a sore throat on one side, how each is diagnosed and treated, and the warning signs that mean it is time to see a provider the same day
Yes and it is one of the most common reasons. Tonsillitis is inflammation or infection of one or both tonsils, the two oval pads of lymphatic tissue at the back of your throat. When only one tonsil becomes infected, the result is one-sided throat pain that may feel swollen, raw, or difficult to swallow through.
Symptoms alongside tonsillitis include fever, bad breath, swollen lymph nodes in the neck, and white or yellow patches on the affected tonsil. Viral tonsillitis the most common type typically clears in 7 to 10 days with rest and fluids. Bacterial tonsillitis requires antibiotics; if left untreated, it can progress to a more serious complication.
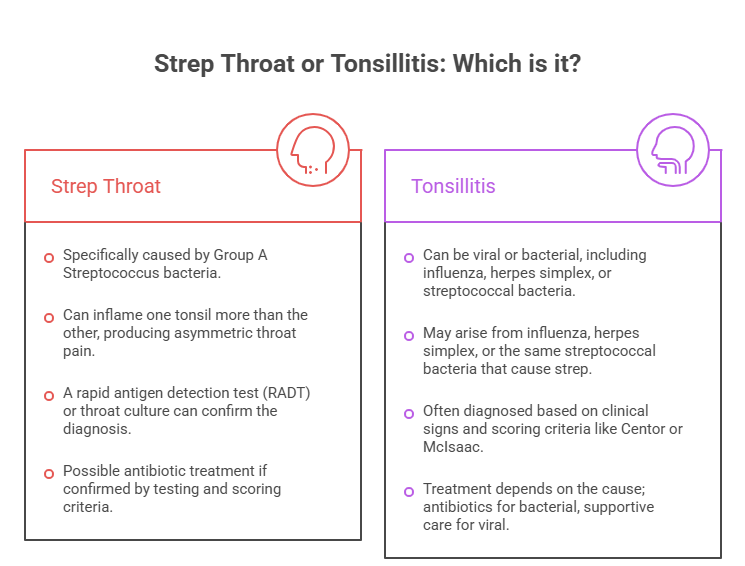
Strep throat is caused specifically by Group A Streptococcus bacteria and can inflame one tonsil more than the other, producing asymmetric throat pain. Tonsillitis, by contrast, can be either viral or bacterial and may arise from influenza, herpes simplex, or the same streptococcal bacteria that cause strep.
The most reliable way to distinguish them is a rapid antigen detection test (RADT), available at urgent care clinics and most primary care offices. Results take under 10 minutes. If the RADT is negative but a provider still suspects strep based on clinical signs, a throat culture can confirm the diagnosis within 24 to 48 hours.
Clinicians often use the Centor or McIsaac scoring criteria to decide whether testing is warranted. This scoring system evaluates four factors: fever, absence of cough, swollen and tender anterior lymph nodes, and tonsillar exudate. A score of 3 or higher typically indicates testing and possible antibiotic treatment. Do not self-prescribe antibiotics overuse contributes to antibiotic resistance and provides no benefit against viral causes.
Related: Sore Throat vs. Strep Throat — Can a Sore Throat Turn Into a Strep Infection?
A peritonsillar abscess (also known as quinsy) is a collection of pus that forms beside or behind one tonsil, almost always affecting only one side. It is the most common deep infection of the head and neck in adults and older teenagers, and it typically develops as a complication of untreated or inadequately treated tonsillitis.
The pain is usually more intense than a standard sore throat and is concentrated entirely on the affected side. It often radiates to the ear on the same side. The abscess may push the affected tonsil toward the center of the throat, causing swelling of the soft palate and uvula.
A peritonsillar abscess does not resolve on its own. Treatment requires drainage of the pus pocket by a healthcare provider, along with a course of antibiotics. At MI Express Urgent Care, our providers can evaluate peritonsillar abscess and coordinate same-day referral when drainage or specialist care is needed.
Post-nasal drip occurs when excess mucus accumulates and drains down the back of the throat, particularly during a cold, sinus infection, or allergy flare. Depending on how the mucus flows, it can irritate one side of the throat more than the other, leading to localized soreness, a persistent tickle, or scratchiness.
This cause is generally less severe than infection-related causes. Symptoms include a feeling of mucus in the back of the throat, a chronic cough, and hoarseness. Treatment addresses the underlying trigger antihistamines for allergies, saline rinses for congestion, or decongestants for sinus-related drainage.
Gastroesophageal reflux disease (GERD) occurs when stomach acid repeatedly flows back into the esophagus and throat. If acid consistently refluxes when a person sleeps on one side, it can irritate that side of the throat more than the other, causing asymmetric soreness.
Laryngopharyngeal reflux (LPR) is a related but distinct condition in which stomach contents reach the larynx and back of the throat without the typical heartburn. LPR often presents with throat clearing, a lump-in-the-throat sensation, hoarseness, and mild one-sided discomfort frequently mistaken for a persistent infection. If you have a one-sided sore throat accompanied by digestive symptoms or no obvious infection signs, GERD or LPR may be the underlying cause and warrants a provider evaluation.
Most one-sided sore throats are not emergencies but certain signs mean you should not wait. Visit MI Express Urgent Care or seek emergency care if you experience any of the following:
At MI Express Urgent Care in Canton and Ann Arbor, we offer rapid strep testing, same-day throat evaluation, and direct referral for specialist care when needed no appointment required. Walk in during clinic hours for prompt assessment.
At an urgent care visit, your provider will examine the throat visually for swelling, redness, exudate, and asymmetry. If strep is suspected, a rapid antigen detection test (RADT) a quick swab of the tonsils can confirm Group A Streptococcus within 10 minutes. A throat culture sent to a lab provides a definitive result if the RADT is inconclusive.
For mild to moderate symptoms without red-flag signs, these evidence-supported home remedies can reduce discomfort while your immune system works:
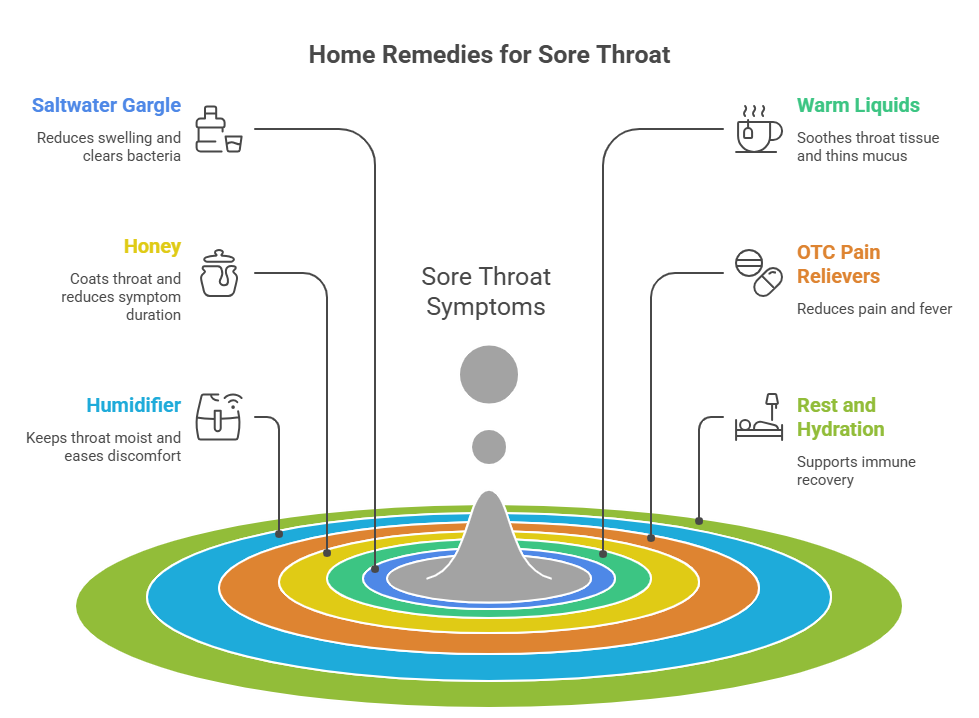
These remedies work well for viral infections, post-nasal drip, and mild irritation. They will not resolve a bacterial infection, peritonsillar abscess, or strep throat; those require medical treatment.
If your throat hurts on one side and you wish to consult an expert, you do not need to look further than MI Express Urgent Care in Canton & Ann Arbor, MI. We have a dedicated team of experienced healthcare professionals who will look into your needs and provide precise and effective treatment options. Contact us today!
One-sided throat pain usually means a single tonsil is inflamed, a lymph node on that side is infected, or a localized condition like a peritonsillar abscess has formed. Unlike a general sore throat, asymmetric pain often points to a specific, identifiable cause worth evaluating.
Yes. Strep throat, caused by Group A Streptococcus, can inflame one tonsil more than the other. A rapid strep test (RADT) at urgent care confirms the diagnosis in minutes and determines whether antibiotics are needed.
Viral tonsillitis typically resolves in 7 to 10 days. Bacterial strep throat usually improves within 24 to 48 hours of starting antibiotics. A peritonsillar abscess requires drainage and may take 1 to 2 weeks to fully resolve.
Yes, if pain is severe, swallowing is difficult, a muffled voice is present, or symptoms last more than a week. MI Express Urgent Care in Canton and Ann Arbor offers rapid strep testing and same-day evaluation no appointment needed.
A peritonsillar abscess causes intense one-sided throat pain, difficulty opening the mouth (trismus), a muffled 'hot potato' voice, drooling, and fever. It requires urgent evaluation and usually needs drainage by a healthcare provider.
A one-sided sore throat lasting more than 2 to 3 weeks warrants medical evaluation to rule out chronic infection, tonsil stones, or in rare cases a tonsillar growth. See a provider if symptoms do not resolve within 10 days.
Yes, though it typically affects both sides equally. Laryngopharyngeal reflux (LPR) can cause one-sided irritation if acid consistently reaches the same area. If there are no signs of infection, GERD or LPR should be evaluated by a provider.




